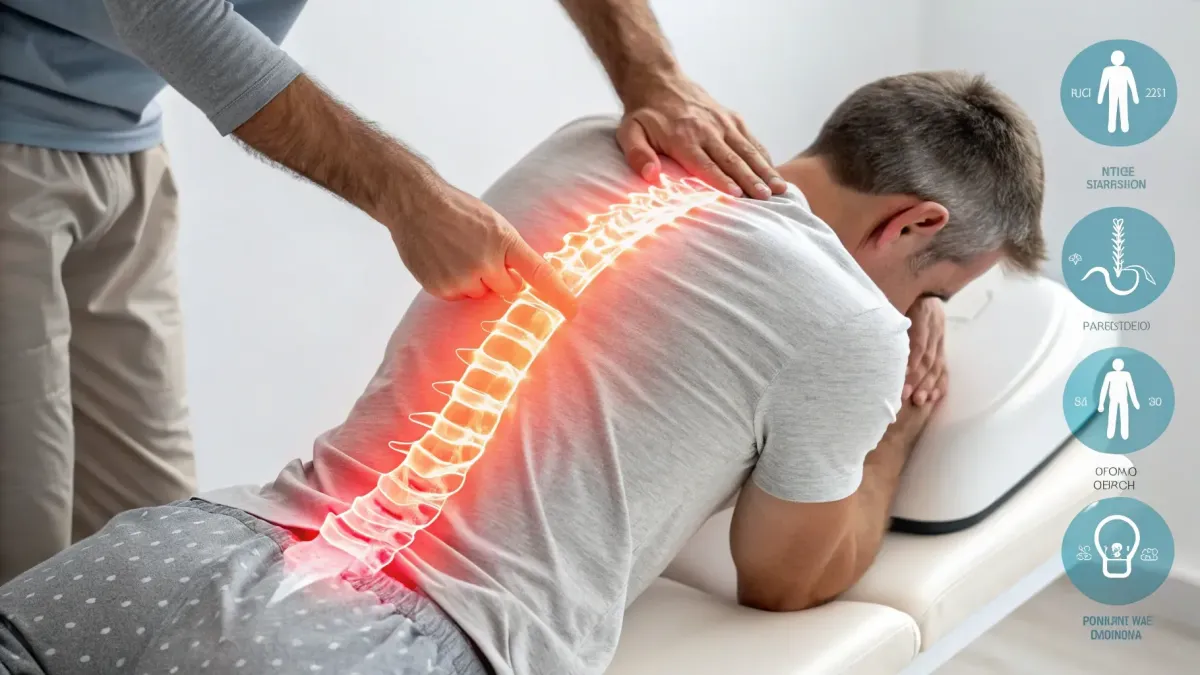
Is stress causing my back pain? How a chiropractic adjustment and lifestyle changes can break the cycle
A growing number of people link stress and anxiety to persistent neck and back pain. This report explains why stress often shows up as musculoskeletal pain, which conservative steps help most, and how targeted care — including a chiropractic adjustment — fits into a practical, evidence-based plan to restore function and reduce flare ups.
Table of Contents
🔍 Why stress shows up as pain
When stress becomes chronic, the body repeats the fight-or-flight response. Repeated activation elevates stress hormones and tightens the sympathetic nervous system, producing sustained muscle guarding around the neck, shoulders, and lower back. Over time this tightness distorts posture, narrows joint spaces, and increases the production of metabolic waste in muscles — all contributors to persistent pain.
Muscle guarding creates a mechanical problem. A tightened muscle behaves like a shortened rope: range of motion narrows, strength declines, and daily tasks become more stressful. That reduced function then adds emotional stress, creating a self-reinforcing loop that turns an acute ache into a chronic issue.
How the pain cycle develops
Psychological stress can cause muscle spasm and trigger points. Those trigger points refer pain to areas that match nerve pathways, making it harder to identify the true source. Postural collapse, often seen when people are tense or fatigued, adds mechanical overload to spinal joints and discs.
"The average human body is 20 percent water and 80 percent stress."
🧠 Practical home steps to interrupt the cycle
Simple, consistent measures can stop escalation before professional care is needed. These include posture focus, basic self-care, and pacing activity.
Ice first, heat later: For new or acute episodes, ice reduces inflammation. Heat is more appropriate for chronic stiffness once acute inflammation has subsided.
Posture awareness: Sitting with the head aligned over the pelvis reduces joint strain. Short, frequent posture checks and ergonomic adjustments lower mechanical stress.
Gentle mobility: Controlled stretching and body-weight movement reduce trigger point activity and ease stiffness.
Short breaks from sitting: Prolonged sitting is strongly linked to lower back pain. Periodic standing and movement restore circulation and muscle balance.
When home measures do not resolve symptoms, targeted clinical interventions — such as a chiropractic adjustment — may be considered to restore joint mechanics and reduce muscle guarding.
💪 Exercise, nutrition, and mind-body tools
Addressing stress requires both physical and psychological approaches. Exercise delivers endorphins, improves muscle endurance, and improves sleep quality. Even brief aerobic activity has measurable benefits for mood and pain perception.
Nutrition matters: Diet influences systemic inflammation. An anti-inflammatory, Mediterranean-style diet rich in vegetables, fruits, whole grains, olive oil, nuts, fatty fish, and minimal processed foods helps lower inflammatory markers and can reduce chronic pain intensity.
Mindfulness-based stress reduction: Techniques such as breathing exercises, body scan meditation, walking meditation, and yoga are practical tools that reduce central nervous system hyperarousal. Regular practice improves emotional regulation and reduces the physiologic drivers of muscle tension.
🛌 Sleep, mattress choice, and daily recovery
Sleep loss amplifies pain sensitivity and weakens coping resources. Aim for consistent 7 to 8 hours nightly. Mattress selection is personal, but the best mattress keeps the spine neutral during sleep. A medium-firm surface that supports the natural curvature of the spine typically works well for many people.
Daily recovery also includes scheduled rest periods, hydration, and avoiding long periods of static posture while working from home or commuting.
🩺 When professional care is needed and what to expect
Many people improve with conservative measures, but persistent or escalating symptoms deserve professional assessment. Clinicians differentiate pain generators — muscle, joint, disc, or nerve — and match treatment to the cause. The most commonly recommended conservative options are:
Physical therapy for mobility, core stabilization, and postural reeducation
Manual therapies, including a chiropractic adjustment, spinal mobilization, and soft tissue techniques
Acupuncture and therapeutic massage for trigger points and muscle release
Interdisciplinary care that includes nutritional guidance and mental health support
The term chiropractic adjustment describes hands-on or instrument-assisted techniques designed to restore joint movement and reduce nerve irritation. Adjustments may be combined with low-force tools such as an activator, or performed on specialized tables that gently distract spinal segments to reduce disc pressure. These approaches can relieve mechanical pain, reduce muscle guarding, and improve function.
Recent research supports using manual therapies alongside exercise and education. Military studies and large medical organizations now recognize that a combination of conservative care that includes a chiropractic adjustment can reduce pain and limit reliance on high-risk pain medications.
⚠️ Red flags that require urgent evaluation
While most pain is mechanical and manageable, urgent medical attention is required for:
Fever with back pain
Saddle anesthesia or loss of bowel or bladder control
Progressive motor weakness or rapidly worsening numbness
Severe unrelenting pain that prevents function despite conservative care
❓ FAQ
Are medications recommended for stress-related muscle pain or anxiety?
Medications can be appropriate depending on the diagnosis. Muscle relaxants, short courses of anti-inflammatory medication, or medications for anxiety and depression may be prescribed after clinical evaluation. Nonpharmacologic measures are preferred first-line and a mental health referral is often considered if symptoms are severe or persistent.
Does insurance typically cover chiropractic care?
Many insurance plans, including Medicare and common commercial carriers, cover conservative spine care such as chiropractic services and physical therapy. Coverage varies by plan and network.
My knee pops but does not hurt. Is that concerning?
Painless popping is usually benign and often due to gas release or minor tracking changes. Pain, swelling, instability, or functional limitation would warrant an assessment and possibly imaging or a focused rehabilitation program.
Is a firm mattress better for back pain?
Mattress preference is individual. A medium-firm mattress that maintains neutral spinal alignment is a good general recommendation. Trial periods and testing different surfaces help identify the best option for each person.
Are telemedicine visits available for back and neck complaints?
Yes. Telemedicine works well for initial history, follow-up, and guided exercise instruction. An in-person visit is recommended for hands-on assessment when needed.
Can care help someone who has rheumatoid arthritis plus anxiety and neck pain?
Yes. People with autoimmune conditions often benefit from a personalized plan that includes medical management, guided physical therapy, lifestyle modifications, and mental health support. Soft tissue work and gentle mobility are typically introduced carefully with monitoring.
What causes waking numbness in the hands, and could it be related to neck pain?
Waking numbness can be caused by peripheral nerve entrapment such as carpal tunnel syndrome, cervical nerve root compression, or both. A clinical evaluation differentiates the source and directs targeted treatments.
🔚 Final summary
Stress often shows up as back and neck pain through sustained muscle tension, postural collapse, and increased inflammation. A combination of self-care, lifestyle change, and targeted clinical treatments can interrupt the pain cycle. Conservative care that includes exercise, mindfulness, nutrition, and manual therapies — including a chiropractic adjustment when appropriate — helps most people avoid escalation to invasive treatments and regain the function needed for daily life.
